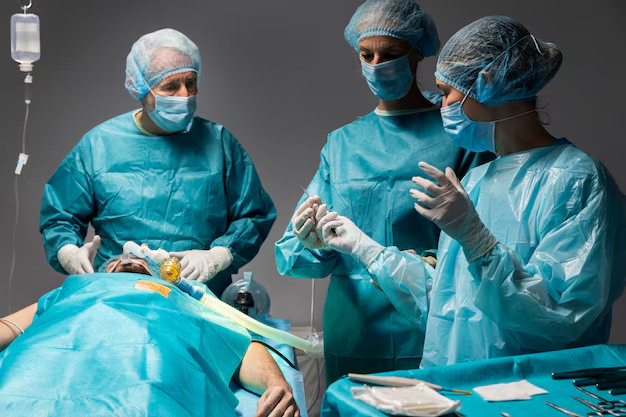
Introduction to the Surgical Team
The surgical team plays a fundamental role in the success of modern medical procedures, acting as a cohesive unit where collaboration and communication are paramount. This team typically comprises various professionals, each with distinct responsibilities that contribute to patient safety and surgical efficacy. The primary members of a surgical team include the surgeon, surgical assistants, anesthesiologists, nurses, and technicians, all working in concert to ensure that procedures are carried out smoothly and effectively.
The surgeon is often the most recognized figure within the surgical team, providing expert knowledge and leadership throughout the operation. Their skills and decisions directly impact the outcome of the procedure. Supporting the surgeon, surgical assistants play a crucial role in facilitating tasks, managing instruments, and anticipating the needs of the operating surgeon. Anesthesiologists, on the other hand, are responsible for the patient’s sedation and monitoring vital signs to ensure safety throughout the procedure. This specialized focus highlights the importance of having dedicated professionals in each role.
The circulating nurse and scrub nurse are also integral to the surgical environment, ensuring that the operation runs without hitches. The circulating nurse coordinates the overall operation by managing supplies and communicating with other staff, while the scrub nurse assists directly with the surgical field, maintaining sterility and providing instruments as required. Each of these roles underscores the significance of teamwork, as the success of a surgical procedure hinges not just on the surgeon’s skills, but also on effective collaboration among all team members.
Recognizing the intricate dynamics of the surgical team is essential, as each member significantly contributes to the overall success of the procedure. In the following sections, we will delve deeper into the specific roles and responsibilities of each team member, illustrating their importance in modern surgical practices.
Key Roles in a Surgical Team
The surgical team comprises various professionals, each with a specific role that is essential for the successful execution of surgical procedures. At the forefront is the surgeon, who possesses the specialized skills required to perform surgeries. Surgeons are responsible for planning the surgical procedure, making crucial decisions during surgery, and ensuring overall patient safety. Their expertise in anatomy, physiology, and surgical techniques makes them indispensable in the operating room.
Assisting the surgeon is the surgical assistant, often a first assistant during the operation. This role may be filled by a physician’s assistant or a surgical technologist. Surgical assistants provide critical support, such as maintaining a sterile environment, handling instruments, and anticipating the surgeon’s needs. Their familiarity with surgical processes enhances the efficiency and effectiveness of the surgery, ensuring the timely and safe completion of the procedure.
An essential member of the surgical team is the anesthesiologist, who is responsible for the patient’s anesthesia and pain management. This role involves evaluating the patient’s medical history, selecting the appropriate anesthetic agents, and monitoring the patient’s vital signs throughout the surgery. The anesthesiologist’s expertise is vital for patient comfort and safety, as they manage potential complications that may arise during anesthesia administration.
Nurses, particularly perioperative nurses, also play a significant role in the surgical team. They are actively involved in preoperative assessments, patient education, and organizing the surgical environment. During the surgery, nurses assist in maintaining sterility and providing essential support to both the surgeon and the anesthesiologist. Their ability to communicate effectively with the entire team is crucial, as they facilitate coordination among team members, further promoting a seamless and patient-centered surgical experience.
Importance of Communication and Coordination
Effective communication and coordination among surgical team members constitute the backbone of modern surgical practice. The intricate nature of surgical procedures demands seamless collaboration, as even minor miscommunications can lead to significant errors and adverse patient outcomes. Proper communication protocols facilitate a shared understanding of each team member’s roles and responsibilities, which is crucial for ensuring that every detail of the surgical plan is accurately executed.
Preoperative briefings serve as a foundational step for fostering communication. During these sessions, the surgical team can discuss the patient’s medical history, surgical objectives, and specific challenges that may arise. This exchange allows each member—from surgeons to anesthetists to nurses—to express any concerns or insights, thereby cultivating a proactive approach to potential complications. Establishing this level of understanding minimizes misunderstandings and lays the groundwork for a cohesive surgical environment.
Intraoperative discussions are equally vital, as they allow for real-time adjustments during the procedure. When unexpected situations occur, open lines of communication enable the team to adapt promptly and effectively, ultimately enhancing patient safety. The ability to communicate candidly under pressure empowers each team member, promoting an atmosphere of shared responsibility that is critical during surgery.
Postoperative debriefings hold significant importance as well, allowing the team to reflect on the procedure. These discussions provide an opportunity to identify any errors, celebrate successes, and explore areas for improvement. By establishing clarity about what transpired, the surgical team can enhance their coordination for future cases, thereby improving overall surgical efficiency and patient care.
Ultimately, robust communication and coordination among surgical team members contribute to creating a culture of safety and high-quality care. This emphasis on collaboration not only safeguards patient outcomes but also fosters professional development and satisfaction within the surgical team.
Training and Continuous Professional Development
The intricate nature of modern surgery necessitates a comprehensive training framework for all members of the surgical team, from surgeons to nurses and anesthetists. Initial education is grounded in rigorous academic programs, typically beginning with a bachelor’s degree in a related field, followed by specialized medical or nursing education. For surgeons, this journey culminates in a residency program, which provides hands-on experience and mentorship in various surgical disciplines. Nursing professionals often pursue additional certifications, such as those offered by the American Association of Critical-Care Nurses, to enhance their expertise in perioperative care.
However, the learning process does not conclude with formal education. Continuous professional development (CPD) is crucial for all surgical team members to stay abreast of evolving surgical techniques and innovations in technology. Hospitals and medical institutions frequently provide opportunities for CPD, such as workshops, seminars, and online courses. Moreover, participation in professional organizations, like the American College of Surgeons, facilitates access to the latest research and resource materials that can significantly improve clinical practice.
Simulation training has emerged as a pivotal component of this ongoing education. By utilizing high-fidelity simulations, surgical teams can practice complex procedures in a risk-free environment. This method not only enhances individual skills but also promotes teamwork, communication, and decision-making under pressure, which are critical in actual surgical settings. Collaborative practice environments, where interdisciplinary teams work together, further foster a culture of shared knowledge and continuous improvement. Such training initiatives have demonstrated a positive impact on patient outcomes, reducing errors and improving overall safety.
In conclusion, the meticulous training and unwavering commitment to professional development among surgical team members are vital to the delivery of high-quality patient care. By ensuring that all team members are equipped with up-to-date skills and knowledge, the surgical field can continue to advance, ultimately enhancing patient safety and surgical outcomes.